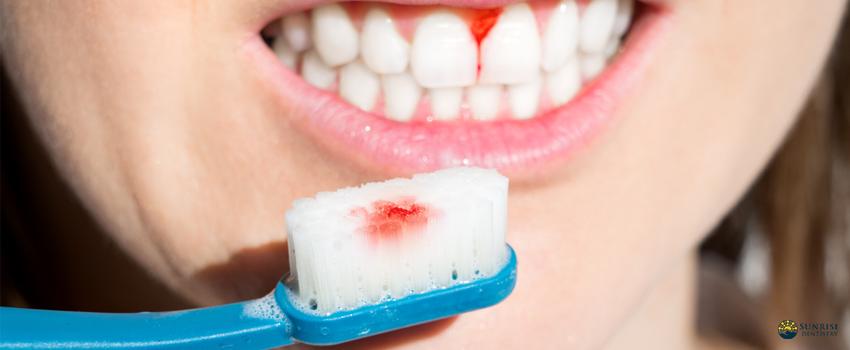
Gum disease is one of the most common oral health problems among adults. A recent Centers for Disease Control and Prevention (CDC) report reveals that over 47% of adults 30 years and above have periodontal disease. It also only becomes more common with age, with 70% of older adults experiencing it.
However, it’s one of the easiest to prevent. Let’s learn more about gum disease, its signs and symptoms, treatment, and prevention.
What is gum disease?
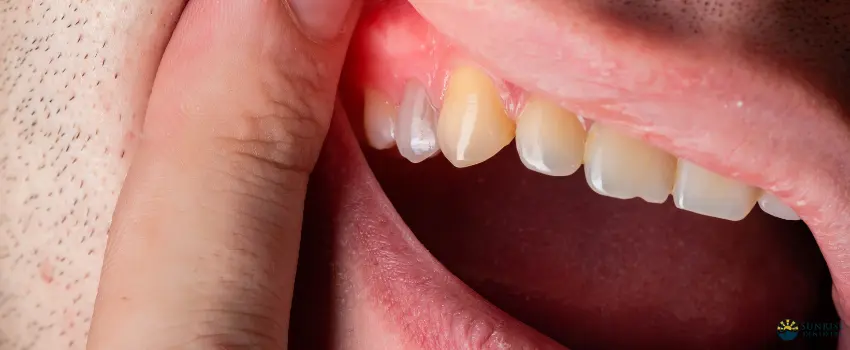
Gum disease is an infection that progressively worsens over time. The early stage of gum disease, called gingivitis, is characterized by swollen and bleeding gums. However, only a few people experience symptoms, especially if they don’t visit their dentist regularly.
Periodontitis is an advanced form of gum disease. In this stage, the inner layer of the gums pulls away from the teeth and forms pockets. It eventually leads to bone and tooth loss.
Gum Disease: Signs and Symptoms

Healthy gums are firm, fit snugly around teeth, and are pale pink-colored. Gum problems such as gum disease can result in the following symptoms:
- Bright red, dusky red, or purplish gums
- Swollen or puffy gums
- New spaces between teeth
- Gum bleeding
- Tender and sensitive gums
- Persistent bad breath
- A change in the way your teeth fit together when you bite
- Loose teeth
- Receding gums
Causes of Gum Disease
Harmful bacteria in your mouth are the leading cause of gum disease. They produce toxins and acids that irritate your gum tissues and weaken teeth enamel. Failing to remove these bacteria with brushing and flossing results in plaque formation. Over time, this can harden into tartar that requires professional cleaning to remove.
Gum Disease: Risk Factors

Several risk factors contribute to plaque and tartar formation, increasing the likelihood of gum disease and other gum problems. These include:
Poor Oral Health Habits
Not brushing or flossing your teeth allows plaque and food debris to remain on and between your teeth. This creates a favorable habitat for harmful bacteria to grow. Plaque will quickly accumulate and harden into tartar over time, eventually leading to gum disease.
Tobacco Product Use
Smokers often develop more plaque and can reduce oxygen levels in the bloodstream, impeding infected gums from healing. This makes gum disease progress more rapidly.
Medications That Cause Dry Mouth
Some medications can reduce saliva production and dry out the mouth. Saliva helps flush out harmful bacteria from the mouth and helps maintain the gums’ protective mucus membrane layer. Without it, your gums and teeth are more vulnerable to gum disease and decay.
Genetics
Recent studies suggest that genetics play a role in gum disease. Some individuals may have a more pronounced immune response to the bacteria that cause periodontal disease.
Recreational Drug Use
Some drugs cause dry mouth, increasing the risk of gum problems. Some, like cocaine, are rubbed over the gums, which can cause gum and bone ulcerations. Drug dependence and abuse can also lead someone to neglect their oral health, increasing the risk of other dental problems.
Inadequate Nutrition
People who don’t eat a healthy diet are at a higher risk for gum disease and other oral health conditions. Starchy, sticky, and sweet foods and drinks only feed the harmful bacteria in the mouth, allowing them to cause more harm to your teeth and gums. Additionally, a poor diet doesn’t give your body the nutrients it needs to heal and be strong and healthy.
Stress
Stress can often lead to teeth grinding and clenching, which puts pressure on the teeth and gums. A study also suggests it may also affect the immune system. People may also forget to care for their oral health during extreme stress.
Gum Disease: Treatments

Good oral hygiene practices are essential to gum disease treatment. Patients who smoke should quit smoking. This may be challenging, but you can always ask your dentist or doctor for help creating an effective cessation plan that suits your needs.
Other gum disease treatment strategies include:
Professional Cleaning
Many non-surgical deep-cleaning techniques help eliminate plaque and tartar to prevent gum irritation. Scaling and root planing removes plaque and tartar from above and underneath the gum line and smoothens the rough spots on the teeth’s surfaces that bacteria can stick to. Dentists may also use lasers to remove tartar with less discomfort and bleeding than root planing.
Medications
Dentists also prescribe medications that can help treat gum disease. After root planing, they can insert timed-release antiseptic chips that contain chlorhexidine or antibiotic microspheres with minocycline into pockets. They may also recommend chlorhexidine-based antiseptic mouthwash to disinfect your mouth.
They also prescribe oral antibiotics to treat persistent gum inflammation.
Surgery
Surgical treatment may be necessary in severe cases of gum disease with gum or bone loss. Periodontists can perform several gum surgery procedures, such as:
- Flap surgery – Periodontists lift back the gums to remove plaque and tartar from deeper pockets. They then suture the gums back in place to fit snugly around the tooth.
- Graft surgery – Graft surgery is useful for cases where the teeth and jaw are too damaged to heal. Gum graft surgeries involve using tissues from the roof of the mouth to cover exposed tooth roots, helping prevent further gum and bone loss. Bone grafts start similar to flap surgery but include adding a bone graft to stimulate the regeneration of any lost jawbone.
- Dental crown lengthening – Crown lengthening procedures reshape gums and bone tissue to expose more teeth. They may be necessary before some cosmetic or restorative dental procedures.
How To Prevent Gum Disease

Practice good oral hygiene.
Maintaining a good oral hygiene regimen is one of the best ways to prevent gum disease. Good oral habits help create an unfavorable environment for the harmful bacteria that cause gum disease to thrive.
Brush your teeth for at least two minutes twice daily, preferably in the morning and before bed. You should also floss your teeth at least once daily; flossing before brushing removes food particles and bacteria that your toothbrush might miss.
Quit smoking.
Aside from giving you bad breath, smoking slows down healing, which makes it more difficult for your gums to heal and fight infections like gum disease.
Go for regular dental visits.
Regular dental visits for professional cleanings every six to twelve months are also important in preventing gum disease. This is more important if you have risk factors that increase the likelihood of developing gum disease, like smoking, dry mouth, and medications. You may need to have professional cleanings more frequently.
Key Takeaway
Gum disease is a common dental problem that can cause several oral health issues, from bleeding gums to tooth and bone loss. Certain factors, such as poor oral hygiene, tobacco use, genetics, and health conditions, increase your risk of gum disease.
Early treatment is vital to prevent it from worsening. Prevent gum disease by practicing good oral hygiene, eating a healthy diet, quitting smoking, and visiting your dentist regularly.
Keep gum disease at bay.
Regular visits to our Pagosa Springs dentist are the best way to avoid or prevent gum disease. Aside from professional cleanings, we also practice holistic dentistry to improve your dental and overall health.
Don’t let gum disease get the best of you. Call Sunrise Dentistry today.