Dental Sleep Medicine in Durango, CO
Dental Sleep Medicine And Oral Appliances For Treating Sleep Apnea
How Do I Find Out If I Have Sleep Apnea?
The first step in diagnosing sleep apnea is to see your dentist, who can tell you if you may be at risk by examining your tongue and teeth. If you have been told or know that you snore at night or you have been observed gasping or choking while sleeping, the chances are likely that you may have sleep apnea. At Sunrise Dentistry, we offer a free sleep consultation in which we will screen you for the degree of sleepiness you have throughout the day, the observance of dental symptoms, the size of your neck, and an analysis of your nasal and oral airway. If the consultation indicates that you are at medium or high risk of having a sleep-breathing disorder, we will recommend that you take an overnight sleep study, which is then analyzed by a doctor of sleep medicine who will return a diagnosis and prescription, if necessary, based on your test results.
At Sunrise Dentistry, we screen our patients for Sleep Wellness and provide dental sleep medicine in Durango, CO. What this means is we look for common attributes that indicate potential sleep disorders, such as sleep apnea. Some of those attributes include the size of the tongue, clenching, bruxism (otherwise known as grinding), and scalloped tongue, which is the result of the tongue thrusting in an effort to keep the airway open while sleeping. The size of the neck and the amount of loose skin between the chin and the neck, also known as turkey wattle, is often a common physical attribute that may indicate an apneic tendency. In fact, people who have a cricomental space (turkey wattle) larger than 1.5 cm and who also have a larger-than-average tongue and an overbite are 95% more likely to be suffering from sleep apnea.
At Sunrise Dentistry, we offer a free consultation for our existing patients.
If you are not an existing patient, we do need to do an exam and take x-rays or see current ones from your dentist. Then, the sleep consultation is free.


Why Should I Be Screened For Sleep Apnea?
We provide dental sleep medicine in Durango, CO. At our office, your overall health, not just your dental health, is very important to us. Dr. Strietzel uses an oral appliance to treat his sleep apnea, and as he learned more about the condition and its risks, he realized that our patient’s first line of defense is a visit to the dentist. Dentists are trained to recognize conditions in the mouth that are often indicators of obstructive sleep apnea (OSA), and he feels that it is important for our patients to know if they are at risk, so they can protect their health.
Untreated OSA can take 12-15 years off your life, and even more if you are a smoker. Many potentially life-threatening conditions, such as cardiovascular disease, high blood pressure, diabetes, and stroke, can be exacerbated by the decreased levels of oxygen created by sleep apnea. And we must ask ourselves, how much do sleep disorders and oxygen deprivation contribute to a healthy person developing these illnesses?
If you have excessive sleepiness during the day, this can be an indicator that your sleep is being compromised, and for the sake of your health, you owe it to yourself and your loved ones to be screened. You are several times more likely to have a car accident and are 23.3% more at risk of a heart attack if you do not seek dental sleep medicine in Durango, CO.
What Are My Options If I Am Diagnosed with Sleep Apnea?
If you’re diagnosed with sleep apnea, Sunrise Dentistry can provide you with suitable dental sleep medicine in Durango, CO.
Here are some treatment options for sleep apnea:
There are several different kinds of surgeries that have been used to treat sleep apnea.
This procedure removes the uvula and tissue from the soft palate and is one of the more common surgeries used to treat obstructive sleep apnea (OSA). It may result in difficulty swallowing long-term and can be excruciating.
The surgeon actually removes a section of the tongue.
A screw is placed into the mandible, and then the tongue is tied forward and attached to it. 55% effective and can affect speech and swallowing.
A laser procedure that reduces tongue size.
Pillar-like inserts are placed in the soft palate to prevent the tissue from vibrating and collapsing against the tongue. This procedure is only effective if the soft palate is where the airway obstruction originates, and it can take several months to become effective.
An electrode is implanted and delivered radio frequency waves to burn excess tissue, creating a larger airway. The procedure has been known to eventually relapse and is only effective when used to treat the mildest forms of OSA.
Moves the upper and lower jaw forward, creating a larger airway. This surgery is the most extreme option and is usually reserved for patients with a severe diagnosis for whom other treatments have failed or for patients with deformed jaws.
These surgeries can cost tens and thousands of dollars and cause significant discomfort and pain. Not all surgeries can be used for any degree of severity of the sleep apnea being treated. There are also high incidences of some surgeries not remaining effective over time.
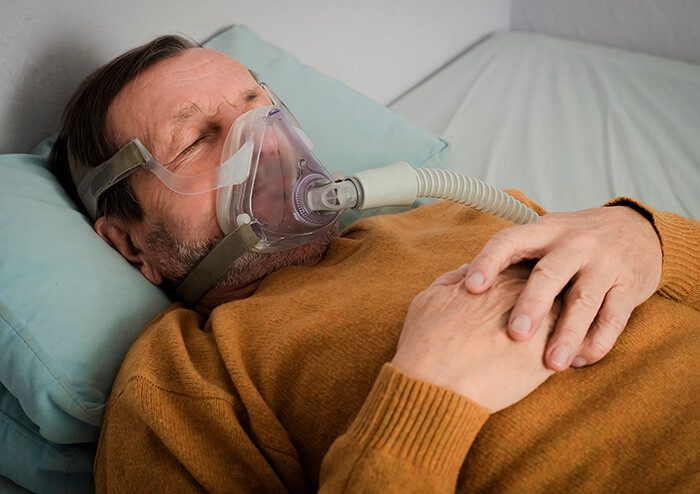
CPAP BiPAP Therapy
CPAP and BiPAP therapy are considered the gold standards for treating sleep apnea overall. It is what we would recommend if a patient is diagnosed with severe sleep apnea unless a patient cannot tolerate the usage of the CPAP, in which case an oral appliance or surgery is better than non-compliance to CPAP treatment. CPAP works by pushing constant air pressure through the nose and into the throat, basically pushing open the airway. The air pressure is adjusted based on the severity of sleep apnea.
BiPAP therapy is similar to CPAP therapy. The difference is that BiPAP increases pressure during the inhale and reduces pressure partly during the exhale. Many people who are not tolerant of the CPAP can be more tolerant of the BiPAP for this reason, especially those who need stronger air pressure.
Oral Appliances
At Sunrise Dentistry, we offer dental sleep medicine in Durango, CO. The treatment we provide in our office for sleep apnea is called a mandibular advancement splint. This is an oral appliance that holds your mouth open slightly and protrudes your chin slightly forward, resulting in opening the airway. We use precision tools in our office in order to determine the proper position to create a mold to make the oral appliance, which is custom-fitted to what works for you.
According to a study report from August 2016 (Trends in CPAP adherence over Twenty Years of Data Collection: A Flattened Curve) posted in The National Library of Medicine, over a 20-year time frame of the study, it was concluded that C-pap compliance is 54% and does not appear to be improving with time. Oral appliances are at a compliance rate of about 70%. Appliances are up to 90% effective and are easy to travel with, use, and clean. If you have been clenching and grinding, the appliance protects you from further damage being caused, serving as a night guard. It also significantly, if not completely, suppresses snoring.
For those who enjoy overnight outdoor activities such as camping and backpacking, our dental sleep medicine in Durango, CO, allows you to maintain this active outdoor lifestyle, as no electricity is necessary.
Oral appliances, however, may not work for everyone. Some people cannot protrude their lower jaw forward enough to find an effective position for treatment. Patients with TMJ may not be able to use an oral appliance as it may aggravate the condition. In cases where oral appliances are not suitable, our team will recommend other types of dental sleep medicine in Durango, CO.



Contact Sunrise Dentistry for Top-Notch Durango Dental Sleep Medicine
If you need Durango dental sleep medicine, look no further than Sunrise Dentistry.
For inquiries regarding our dental sleep medicine in Durango, CO, don’t hesitate to reach out. We’ll be more than happy to help you improve the quality of your sleep. Give us a call today!


